Why do I need an angiogram?
These are the common reasons why your doctor may recommend that you have a coronary angiogram:
- Symptoms of coronary artery disease, such as chest pain (angina)
- Pain in your chest, jaw, neck or arm that can not be explained
- A heart defect you were born with (congenital heart disease)
- Heart failure symptoms (shortness of breath, ankle swelling)
- Other blood vessel problems or a chest injury
- A heart valve problem that requires surgery
- New or increasing chest pain (unstable angina)
- Symptoms of a heart attack (Sudden onset of chest pain)
You may also need an angiogram if you are going to have surgery unrelated to your heart. This may be because you are at a high risk of having a heart problem during that surgery.
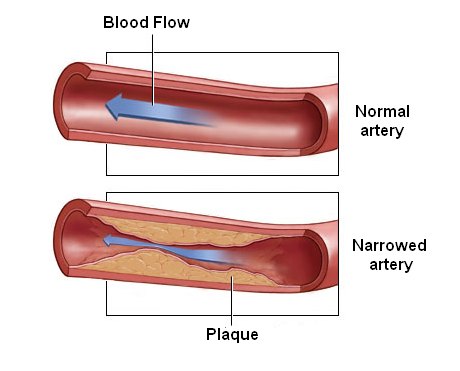
The physician doing the procedure will be looking for any blockages or narrowing in your heart arteries. Blockages or narrowing may explain your symptoms. Coronary Artery Disease (also called CAD) is the most common type of heart disease. It is also the leading cause of death for both men and women in Canada.
Coronary artery disease occurs when cholesterol plaque builds up in the arteries. This build up results in the heart not getting enough of the blood and oxygen it needs to work well. Over time, this can weaken or damage the heart. If a plaque splits or breaks, the body tries to fix this by forming a blood clot around it. The new clot can block blood in the artery and stop blood flow to the heart. This is a common cause of a ‘heart attack’.
Are there any other less invasive tests for my condition?
There are other tests and you may have already had some of them before your referral for the angiogram. These tests include:
- Exercise Treadmill Test (ETT) or stress test
- Nuclear Test or MIBI scan (with or without exercise)
- Echo or Stress ECHO (Heart Ultrasound) test
- Computed Tomography Angiogram (also known as a CTA or “CAT” scan)
The common tests listed above provide different kinds of information. However, the angiogram is generally the most accurate way to confirm coronary artery disease.
What are the risks of an angiogram?
Angiograms are ‘invasive’ procedures and there are some risks. Potential risks and complications can include:
- Hematoma (blood under your skin or a bruise) is the most common complication after an angiogram. Most hematomas generally resolve one to two weeks after an angiogram.
- Irregular heartbeat (arrhythmia) – this is sometimes caused by the catheters within the heart or the X-ray dye/contrast injection. This usually settles by the end of the procedure.
- Allergic reaction to the X-ray dye/contrast happens in 1 per 100 people who have an angiogram. Medicines are available to help treat this. If you have a known allergy to X-ray dye: let our procedure booking team and your nurse on the day of the procedure know.
- Heart attack or stroke – very rarely, the tip of the catheter can dislodge a blood clot or fatty plaque from the wall of your blood vessel. There is a risk that one of these clots may block the blood supply to your heart or brain and trigger a heart attack or stroke. This happens in less than 1 in 1,000 people.
- Death. This is very rare and happens in less than 1 in 1,000 people during or after an angiogram. The risk is increased in people who already have other medical conditions, such as problems with their lungs or kidneys.
- Other uncommon complications include kidney damage due to the X-ray dye, bleeding from the puncture site, infection at the puncture site, and radiation exposure.
Major complications are rare and your doctor will discuss the risks applicable to your case prior to asking you to sign a consent form for the procedure. Your doctor should only recommend an angiogram if they feel the benefits outweigh the small risk.
Next article: